Families and caregivers can strengthen a Personal Independence Payment (PIP) or Adult Disability Payment (ADP) claim in 2026 by focusing on how a condition affects daily living and mobility rather than the diagnosis itself.
The best PIP and ADP insider tips include keeping a detailed “bad day” diary, understanding the PIP points system, providing evidence that reflects daily struggles, and explaining risks such as pain, breathlessness, falls, or memory problems clearly during assessments.
Recent Personal Independence Payment news today also shows growing concern around new PIP rules, reviews, and the PIP payment increase expected in April 2026. For many claimants, strong preparation and consistent evidence now matter more than ever.

Key PIP and ADP Insider Tips for 2026
- Focus on how the condition affects daily life, not just the medical diagnosis.
- Learn how the PIP points system works before completing the form or attending an assessment.
- Keep a “bad day” diary that records pain, fatigue, falls, confusion, breathlessness, or mobility struggles.
- Explain whether tasks take longer, feel unsafe, or require help from another person.
- Keep copies of every form, letter, and medical document you submit.
- Use real examples when answering PIP assessment questions instead of giving short or vague responses.
- Understand that PIP descriptors and points focus on reliability, safety, and consistency.
- Do not downplay conditions such as anxiety, PTSD, or personal independence payment depression during assessments.
- Caregivers should attend assessments when possible to provide additional context and support.
- Review the latest PIP News regularly, especially updates about the PIP payment increase and new PIP rules for 2026.
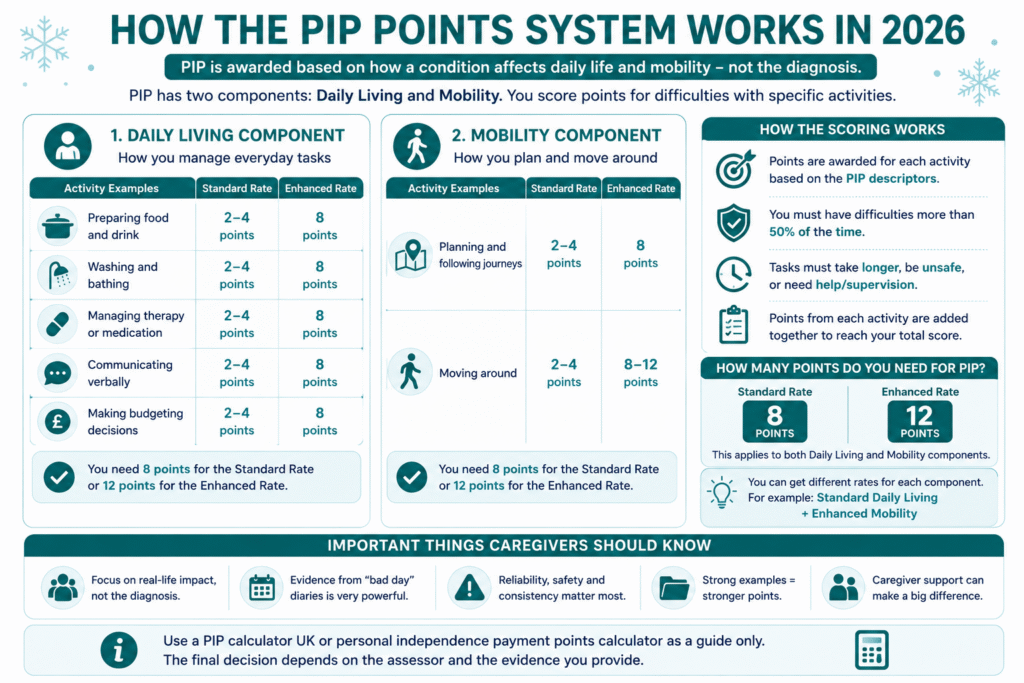
How the PIP Points System Works in 2026
The PIP points system measures how a health condition or disability affects a person’s ability to manage everyday activities safely and consistently. Assessors do not award points based on a diagnosis alone. Instead, they use specific PIP descriptors to decide how much support someone needs with daily living and mobility tasks.
PIP divides assessments into two areas:
- Daily Living
- Mobility
Each section contains activities with different scoring levels. These scores are known as personal independence descriptors or PIP descriptors and points.
For example, the daily living section looks at tasks such as:
- Preparing food
- Washing and bathing
- Managing medication
- Communicating
- Making budgeting decisions
The mobility section focuses on:
- Planning journeys
- Moving around safely
Many caregivers wrongly assume a medical diagnosis automatically qualifies someone for support. In reality, assessors look for evidence that the person cannot complete activities safely, repeatedly, to an acceptable standard, or within a reasonable time, for more than 50% of the time.
This rule becomes especially important for people with fluctuating conditions, chronic pain, mobility issues, anxiety, or personal independence payment depression claims.
How Many Points Do You Need for PIP?
Claimants usually need:
- 8 points for the standard rate
- 12 points for the enhanced rate
This applies separately to both Daily Living and Mobility components.
For example, someone may receive:
- Standard Daily Living
- Enhanced Mobility
depending on their total score.
Many families now use a personal independence payment points calculator or a PIP calculator UK tool to estimate potential entitlement before applying. While these tools help, they cannot replace strong written evidence and detailed examples from daily life.
Caregivers should also understand that PIP mobility points often depend on reliability and safety rather than physical distance alone. Someone may technically walk a short distance but still qualify if pain, fatigue, dizziness, or psychological distress makes the activity unsafe or inconsistent.
RELATED: Scotland PIP ADP Update 2026: What Care Businesses and Claimants Must Know
The Biggest Mistake People Make During PIP Assessments

The biggest mistake claimants make during PIP assessments is talking about their diagnosis instead of explaining how their condition affects daily life.
Many people say things like:
- “I have arthritis.”
- “I suffer from depression.”
- “I have chronic pain.”
However, PIP assessment questions focus on functional impact, not medical labels.
Assessors want to know:
- What happens when you try to cook?
- Do you forget medication?
- Can you walk safely without stopping?
- Does anxiety prevent you from travelling alone?
- Do you need prompting, supervision, or physical support?
This is where many claims lose valuable points.
For example, saying, “I struggle with anxiety,” sounds far weaker than, “I avoid travelling alone because anxiety causes panic attacks, confusion, and severe distress during journeys.”
The second answer directly connects the condition to the PIP descriptors.
Caregivers often notice daily difficulties that claimants forget to mention during assessments. A family member may remember:
- falls in the bathroom
- missed medication
- breathlessness during simple tasks
- confusion with money
- mobility problems after short walks
These details matter because the new PIP points system rewards evidence that clearly shows risk, supervision needs, or inability to complete tasks reliably.
Another major mistake involves downplaying symptoms. Many people try to appear positive or independent during assessments, especially older adults who feel uncomfortable discussing personal struggles. This issue affects many DWP PIP older claimants who have lived independently for years and dislike asking for help.
Unfortunately, statements like:
- “I manage most days”
- “I just get on with it”
- “I try not to complain”
can reduce points if they contradict written evidence.
Instead, claimants should answer honestly and describe what happens on bad days, especially if those difficulties affect them more than 50% of the time.
Caregivers should also encourage claimants to give specific examples rather than short answers. Strong examples make PIP questions easier for assessors to understand and harder to misinterpret.
READ MORE: HICBC Child Benefit Rule Change UK: What Care Workers Need to Know in 2026
Why Caregivers Should Keep a “Bad Day” Diary
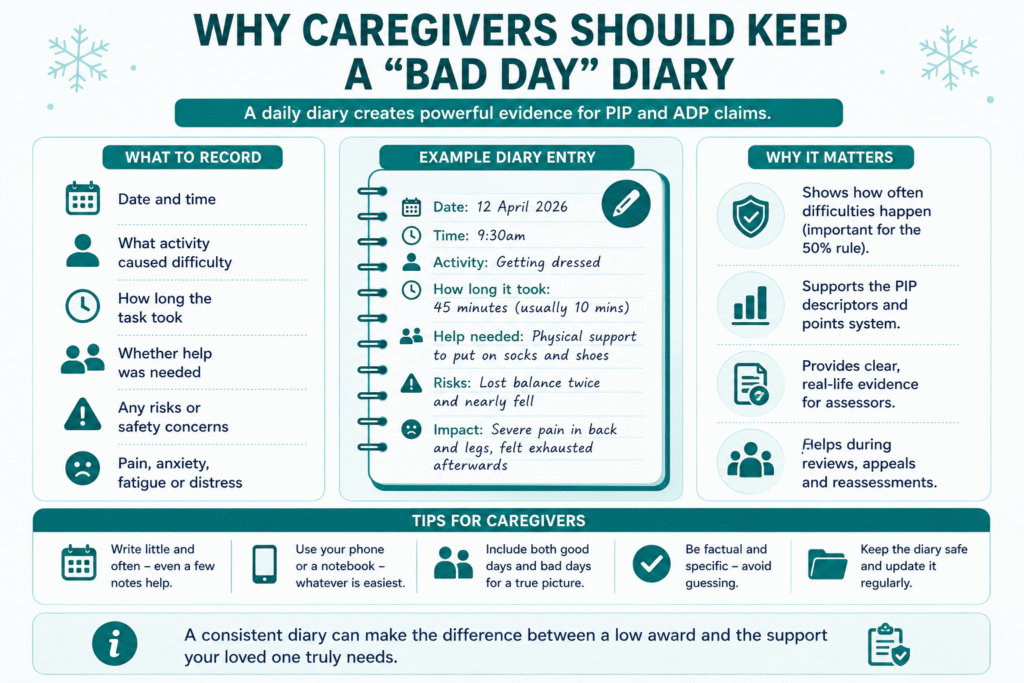
A “bad day” diary can become one of the strongest pieces of evidence in a PIP or ADP claim, especially for people with fluctuating conditions, mental health challenges, chronic pain, or fatigue-related illnesses.
Many claimants forget important details during assessments. Caregivers often remember those moments more clearly because they see the daily impact firsthand.
A diary helps create a clear timeline of:
- falls or mobility struggles
- panic attacks or emotional distress
- missed medication
- confusion or memory problems
- breathlessness
- pain flare-ups
- unsafe situations in the kitchen or bathroom
This type of evidence supports the PIP descriptors and points system because it shows how often difficulties happen in real life.
For example, instead of writing: “My mother struggles with mobility,” a caregiver can document: “On three occasions this week, my mother stopped halfway up the stairs due to breathlessness and knee pain. She needed physical support to continue safely.”
That level of detail carries far more weight during PIP assessments.
A diary also helps caregivers answer pip assessment questions consistently during reviews or reassessments. Inconsistent answers often trigger additional scrutiny, especially when written evidence conflicts with verbal responses.
People with depression, PTSD, anxiety, fibromyalgia, arthritis, or neurological conditions may experience “good days” and “bad days.” A diary helps demonstrate that even if someone appears well occasionally, they still struggle for more than 50% of the time.
Caregivers should encourage claimants to record:
- dates and times
- what activity caused difficulty
- how long the task took
- whether help was needed
- any risks or safety concerns
Even simple phone notes can help build a strong evidence trail over time.
Many families focus heavily on medical records, but assessors often place equal importance on practical daily examples. A detailed diary bridges the gap between a diagnosis and the real-life challenges behind a PIP claim.
SEE ALSO: What Is Pension Age Disability Payment (PADP)? 2026 Update
Latest PIP News: How Much Will PIP Rise in 2026?
The latest PIP News confirms that Personal Independence Payment rates increased again in April 2026 as part of the government’s annual benefits uprating process. Many families searching “How much will PIP rise in 2026” or “How much will PIP be in 2026” want to understand how these changes affect household finances and long-term care planning.
The new PIP rates for 2026/27 mean some claimants now receive up to £778.40 every four weeks, depending on their award level and eligibility.
Current PIP rates include:
- Standard Daily Living: £73.90 per week
- Enhanced Daily Living: £110.40 per week
- Standard Mobility: £29.20 per week
- Enhanced Mobility: £77.05 per week
These updated figures reflect the latest PIP payment increase introduced in April 2026.
However, caregivers should pay close attention to ongoing discussions around new PIP rules and future assessment reforms. The government continues to review eligibility criteria, assessment processes, and support for long-term conditions. These changes could affect future claims, reviews, and reassessments.
Families supporting vulnerable adults should also monitor Personal Independence Payment news today for updates involving:
- reassessment rules
- mental health claims
- mobility scoring
- support for older claimants
- changes affecting ADP in Scotland
Staying informed helps caregivers prepare stronger evidence and avoid unnecessary stress during reviews or appeals.
MORE: Bank Holiday Early Benefit Payments DWP: May 2026 Update
Useful PIP Contact Numbers and Support Resources
Many caregivers struggle to find the correct PIP phone number when they need urgent help with a new claim, review, or assessment update. Keeping the right contact details nearby can reduce stress and help families respond quickly to DWP requests.
The main personal independence payment phone number for new claims and general enquiries is:
- PIP New Claims: 0800 917 2222
For people managing an existing claim, review, or change in circumstances, the pip contact number existing claim is:
- PIP Enquiry Line: 0800 121 4433
Claimants can use these lines to:
- request forms
- report health changes
- ask about payments
- check assessment updates
- request copies of previous claim forms
Caregivers should also consider getting support from:
- Citizens Advice
- disability charities
- welfare rights advisers
- local carers’ organisations
These services often help families understand pip descriptors, gather evidence, prepare for assessments, and challenge unfair decisions.
People living in Scotland who receive Adult Disability Payment (ADP) can also contact Social Security Scotland for application support and guidance during transfers from PIP.
Before calling, caregivers should keep:
- National Insurance numbers
- appointment dates
- medical evidence
- copies of claim forms
close by to make conversations faster and easier.
Final Thoughts…
Strong PIP and ADP claims rarely succeed because of a diagnosis alone. Successful claims usually include detailed examples, consistent evidence, and clear explanations of how a condition affects daily life.
Caregivers often play a critical role in that process. They notice changes that claimants may overlook, help document difficult moments, and provide valuable support during stressful assessments or reviews.
Understanding the PIP points system, keeping a detailed “bad day” diary, and preparing carefully for pip assessment questions can significantly improve the quality of a claim. Small details matter. Explaining why a task feels unsafe, painful, exhausting, or impossible often carries more weight than medical terminology alone.
Families should also stay updated with the latest PIP News, especially as discussions around new PIP rules and future assessment changes continue throughout 2026.
Most importantly, claimants should never feel pressured to minimise their struggles. Honest, specific, and well-supported answers give assessors a clearer picture of daily challenges and help ensure people receive the support they genuinely need.
Need Support Navigating PIP or ADP?
Care Sync Experts supports caregivers, families, and vulnerable adults with practical guidance on care, compliance, and daily living support.
Whether you need help understanding PIP descriptors, preparing evidence for assessments, or staying updated with Personal Independence Payment news today, our team provides clear and compassionate resources designed for real-world caregiving challenges.
Explore more caregiver support guides and disability benefit resources with Care Sync Experts to stay informed, prepared, and confident throughout the claims process.
FAQ
Is PIP or ADP Better?
Adult Disability Payment (ADP) and Personal Independence Payment (PIP) provide similar financial support, but many claimants in Scotland consider ADP less stressful because Social Security Scotland uses a more compassionate approach during assessments and reviews.
ADP also places greater emphasis on gathering supporting information before requiring face-to-face consultations.
When Did ADP Replace PIP?
Adult Disability Payment began replacing PIP for working-age disabled adults in Scotland in 2022. Social Security Scotland gradually transferred existing PIP claimants from the DWP system to ADP, and all transfers now happen automatically without requiring a new application.
How Often Is ADP Paid?
Adult Disability Payment usually pays every four weeks directly into the claimant’s bank account. In some situations, terminally ill claimants may receive weekly payments depending on their circumstances and support arrangements.
What Are Common PIP Mistakes?
Many people lose valuable points because they:
– downplay their symptoms
– give vague answers during assessments
– focus only on diagnosis instead of daily impact
– forget to mention safety risks or supervision needs
– fail to provide detailed supporting evidence
Caregivers can help avoid these mistakes by keeping records, documenting bad days, and preparing examples before the assessment.
