Working Tax Credit has ended in the UK. You can no longer make a new claim, and HMRC says tax credits ended on 5 April 2025 with no further payments being made. People who qualified for replacement support should have received a letter about moving to Universal Credit or Pension Credit instead.
For care workers, unpaid carers, single parents, and families on low income, the real question in 2026 is no longer, “Can I claim Working Tax Credit?” The better question is, “What support can I claim now while I work, care, or raise children?”.
If you work in care and your income changes because of shifts, overtime, reduced hours, childcare costs, or caring duties at home, you should check your current benefit entitlement rather than rely on old tax credits guidance. Universal Credit has replaced Working Tax Credit for most working-age people, while Pension Credit may apply if you are over State Pension age.
Working families should also check support such as Child Benefit, childcare help through Universal Credit, and any extra help linked to disability, rent, or caring responsibilities.

What Is Working Tax Credit?
Working Tax Credit was a UK benefit that helped people who worked but earned a low income. HMRC paid it to eligible workers, including some single parents, couples, disabled workers, and people without children who met the rules at the time.
Despite the name, Working Tax Credit did not work like a normal tax refund. It was a means-tested payment, which means HMRC looked at your household income, working hours, age, disability status, relationship status, and childcare responsibilities before deciding how much you could get.
So, what is tax credit in this context? A tax credit was financial support from the government to top up income or help with family costs. The old system included Working Tax Credit for low-paid workers and Child Tax Credit for people responsible for children.
Some people also used the phrase in-work tax credit to describe this type of support because it helped people who worked but still struggled with everyday costs.
In 2026, Working Tax Credit no longer supports new or existing claimants. Universal Credit has replaced it for most working-age people who need help with low income, rent, children, childcare, disability, or caring responsibilities.
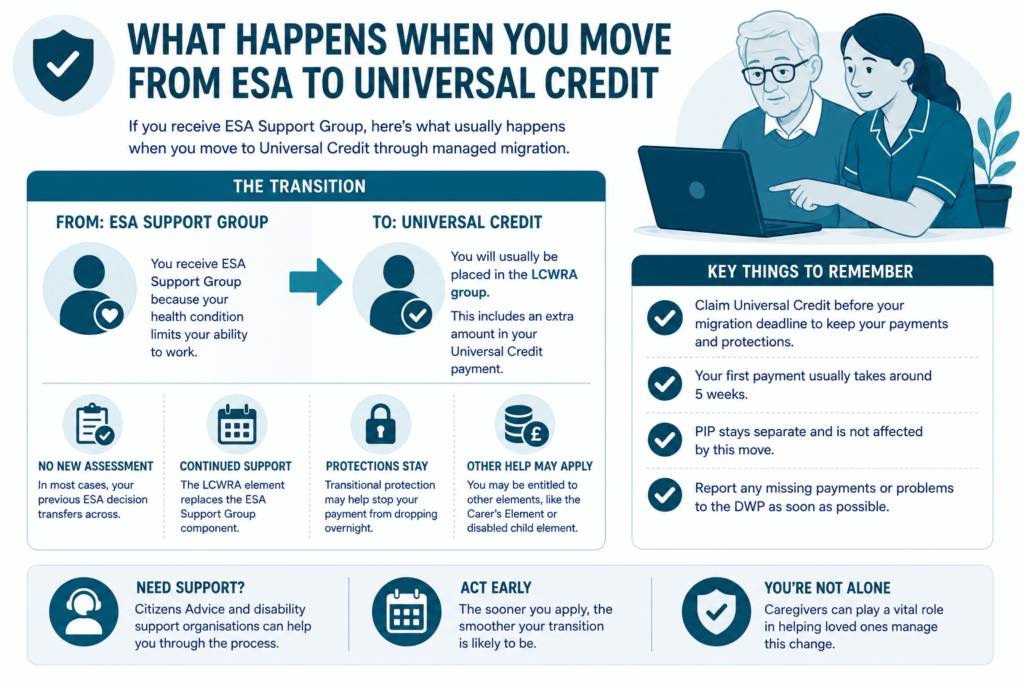
RELATED: Moving From ESA Support Group to Universal Credit: What You Need to Know in 2026
Can You Still Claim Working Tax Credit in 2026?
No. You cannot make a new Working Tax Credit claim in 2026. Tax credits ended on 5 April 2025, and GOV.UK says no more payments will be made. People who qualified for replacement support should have received a letter about moving to Universal Credit or Pension Credit instead.
This means a working tax credit form or old working tax credit calculator can no longer help you start a new claim. If you work on a low income, raise children, pay rent, manage childcare costs, or care for someone, you should now check whether Universal Credit, Child Benefit, Pension Credit, or other support applies to you.
Some people may still need to deal with old tax credit account issues. For example, HMRC may contact you about a final decision, an overpayment, an appeal, or a possible working tax credit refund linked to a period before the scheme ended. GOV.UK still allows people to challenge tax credit decisions or dispute overpayments where relevant.
What Replaced Working Tax Credit?
Universal Credit replaced Working Tax Credit for most working-age people on a low income. Unlike the old tax credit system, Universal Credit can support people whether they work, work part-time, care for someone, look after children, pay rent, or cannot work because of illness or disability.
For working carers and care workers, this matters because income can change from month to month. You may work shifts, accept overtime, reduce your hours to care for a loved one, or pay for childcare so you can stay in work. Universal Credit looks at your circumstances and earnings, then adjusts the amount you receive.
If you are over State Pension age, Pension Credit may apply instead. Some people may also qualify for help with housing costs, council tax support, disability benefits, or Child Benefit depending on their situation.
People often ask, can you get Working Tax Credit without a child? In the old system, some workers without children could qualify if they met the rules. In 2026, that no longer matters because Working Tax Credit has ended. The practical step now is to check what support replaces it for your current circumstances.
READ MORE: What Is the Retirement Age UK for Female Workers in 2026?
What About Child Working Tax Credit and Child Tax Credit?
Many people say Child Working Tax Credit, but the old system had two separate benefits: Working Tax Credit and Child Tax Credit. Working Tax Credit helped low-paid workers. Child Tax Credit helped people responsible for children.
So, what is Child Tax Credit? It was a payment for families with children, based on household income and family circumstances. It could help whether the parent worked or not, but the amount depended on income, number of children, disability needs, and other factors.
People also ask, how much is Child Tax Credit in 2026? The simple answer is that Child Tax Credit has ended, so families cannot make a new claim or receive ongoing payments under the old tax credit system.
If you are a working parent, single parent, care worker, or unpaid carer raising children, you should now check Universal Credit and Child Benefit instead. Universal Credit may include extra support for children, rent, childcare costs, disability, or caring responsibilities, while Child Benefit remains separate from the old tax credits system.
Is Child Tax Credit the Same as Child Benefit?
No. Child Tax Credit and Child Benefit are not the same.
Child Tax Credit belonged to the old tax credits system, which has now ended. It helped families with children based on income and circumstances, but you can no longer make a new claim or receive ongoing Child Tax Credit payments in 2026.
Child Benefit still exists. It pays a weekly amount to someone responsible for a child, usually until the child turns 16, or until 20 if they stay in approved education or training. For the 2026/27 tax year, Child Benefit pays £27.05 per week for the eldest or only child and £17.90 per week for each additional child.
So, if you ask “is Child Tax Credit the same as Child Benefit?”, the answer is no. Child Tax Credit has ended, but Child Benefit continues.
Families often ask, “is Child Benefit going up in 2026?” Yes. GOV.UK lists the 2026/27 weekly rate as higher than the 2025/26 rate, which was £26.05 for the eldest or only child and £17.25 for other children.
SEE ALSO: How to Report Benefit Fraud in the UK (2026)
Support for Single Parents, Working Carers, and Childcare Costs
Single parents, care workers, and unpaid carers often manage more than one responsibility at once. You may work shifts, raise children, care for a loved one, pay rent, and cover childcare before your wages even settle. That is why old Working Tax Credit guidance can confuse families in 2026.
If you are a working tax credit single parent searching for what replaced your support, you should check Universal Credit instead. Universal Credit may include extra help for children, rent, disability, childcare costs, or caring responsibilities, depending on your situation.
If you pay for registered childcare while you work, Universal Credit can cover up to 85% of eligible childcare costs. From April 2026, the maximum monthly amount is £1,071.09 for one child or £1,836.16 for two or more children. You usually pay childcare costs first, report them through your Universal Credit account, and claim the money back.
People also ask, how much benefits does a single parent get? There is no single amount. It depends on earnings, rent, children, childcare costs, disability, savings, and whether you care for someone. A benefits calculator can give a clearer estimate than an old Working Tax Credit calculator.
What Do Gross Pay and Gross Annual Income Mean?
When you check Universal Credit, childcare support, or other benefits, you may need to enter your income details correctly. Two common terms can confuse people: gross pay and gross annual income.
Gross pay means the money you earn before tax, National Insurance, pension contributions, student loan repayments, or other deductions come out. For example, if your payslip shows £2,000 before deductions and £1,650 after deductions, your gross pay is £2,000.
Gross annual income means your total yearly income before deductions. If you work in care, this may include regular wages, overtime, sleep-in shifts, weekend rates, bonuses, or extra hours.
This matters because many benefit checks look at income before or after certain deductions, depending on the support you apply for. If your hours change each month, use the most accurate figures you can. Care workers, single parents, and unpaid carers with flexible or changing income should avoid guessing, because wrong income details can affect payments.
Some people search for a how rich am I calculator UK or a benefits calculator to understand where they stand financially. A proper benefits calculator gives a more useful answer because it looks at earnings, rent, children, childcare costs, disability, savings, and caring responsibilities.
MORE: Individual Support Package: What It Means for Care at Home
How to Check What You Can Claim Now
If you previously searched for a Working Tax Credit calculator, use a current benefits calculator instead. Working Tax Credit has ended, so an old calculator may explain past entitlement, but it will not help you make a new claim in 2026.
Start by checking your age. If you are under State Pension age and work on a low income, Universal Credit may apply. If you are over State Pension age, check Pension Credit instead.
Before you check, gather the details that affect your claim:
- Your gross pay and monthly earnings
- Rent or housing costs
- Number of children you support
- Registered childcare costs
- Disability or health conditions
- Caring responsibilities
- Savings and partner’s income, if relevant
If you still have an old tax credit account issue, contact HMRC about final notices, overpayments, appeals, or a possible Working Tax Credit refund. Do not ignore letters about old tax credits, even though the scheme has ended.
For working carers and families, the safest next step is simple: check your current entitlement based on today’s rules, not the old Working Tax Credit system.
Final Thoughts…
If you work in care, care for a loved one, or raise children on a low income, do not rely on old Working Tax Credit guidance. The scheme has ended, so the right support now depends on your current age, earnings, rent, childcare costs, disability needs, and caring responsibilities.
Working carers often carry pressure quietly. You may support vulnerable people at work, then return home to care for your own family. If your income feels stretched, check what help exists now instead of assuming you do not qualify.
Universal Credit may support working-age people on a low income. Child Benefit may help if you are responsible for a child. Pension Credit may apply if you are over State Pension age. Other support may also apply if you pay rent, have a disability, or care for someone regularly.
The key message is simple: Working Tax Credit has ended, but support for working families has not disappeared. Check your entitlement early, keep your income details accurate, and ask for advice if your situation changes.
Stay Informed About Support for Working Carers
Changes to benefits, tax credits, childcare support, and low-income help can affect care workers, unpaid carers, single parents, and families across the UK care sector.
At Care Sync Experts, we help caregivers, care providers, and care professionals understand the practical changes that matter, from workforce pressures and financial support to compliance, care planning, and everyday care decisions.
Explore more expert guides from Care Sync Experts to stay informed, make confident decisions, and keep up with the issues shaping care work and family support across the UK.
FAQ
What is a tax credit and how does it work?
A tax credit reduces the amount of tax someone owes or increases financial support through the tax system. In the old UK benefits system, Working Tax Credit and Child Tax Credit worked more like means-tested payments than ordinary tax reductions. They helped low-income workers and families, but both ended on 5 April 2025, and no further tax credit payments will be made.
How much was Working Tax Credit in the UK?
Working Tax Credit no longer pays anything in the UK because the scheme has ended. For reference only, GOV.UK lists the previous 2024/25 maximum annual elements as £2,435 for the basic element, £2,500 for the couple or lone parent element, £1,015 for the 30-hour element, £3,935 for the disabled worker element, and £1,705 for the severe disability element. These old rates do not create entitlement in 2026.
Do you get money back from a tax credit?
Sometimes, but it depends on the type of tax credit. In the old UK tax credit system, HMRC could pay support directly to eligible people, but it could also ask for money back if someone received too much.
Since tax credits have ended, some people may still need to finalise old claims, check annual review letters, or deal with overpayments linked to payments made before 5 April 2025.
Can I claim Child Benefit if I earn over £50k in the UK?
Yes. You can still claim Child Benefit if you earn over £50,000. The important threshold from the 2024/25 tax year through 2026/27 is £60,000 for the High Income Child Benefit Charge.
If your adjusted net income is over £60,000, you may have to pay some Child Benefit back through the charge; the charge increases until Child Benefit is fully clawed back at higher income levels. GOV.UK provides a Child Benefit tax calculator to check this.