Sundowning typically starts in the late afternoon, usually between 3 p.m. and 5 p.m., and continues into the evening and night. This pattern often aligns with the time the sun begins to set, so changes in light, like knowing what time is sundown today UK, can influence when symptoms begin.
Sundowning dementia refers to a group of behaviors, such as confusion, agitation, and restlessness, that worsen as daylight fades. While most caregivers notice symptoms in the evening, some individuals may also experience sundowning in the morning, especially when sleep patterns are disrupted.
For caregivers, understanding what time is sundowning helps you anticipate changes in behavior and prepare the environment before symptoms escalate.

Key Takeaways About Sundowning
- What time is sundowning? It usually starts between 3 p.m. and 5 p.m. and can continue into the night.
- Sundowning dementia is not a disease. It is a pattern of symptoms like confusion, anxiety, and agitation that worsen later in the day.
- Symptoms often peak around sunset, especially as lighting changes and fatigue builds.
- What triggers sundowning? Common triggers include tiredness, low lighting (sometimes called night shading), hunger, and disrupted routines.
- Behaviour can become challenging, including restlessness, wandering, or even aggressive dementia episodes in some individuals.
- Early preparation helps. Adjusting lighting, reducing noise, and maintaining a calm routine can reduce symptoms.
- Each person is different. While evening is most common, some people may show symptoms at other times of the day.
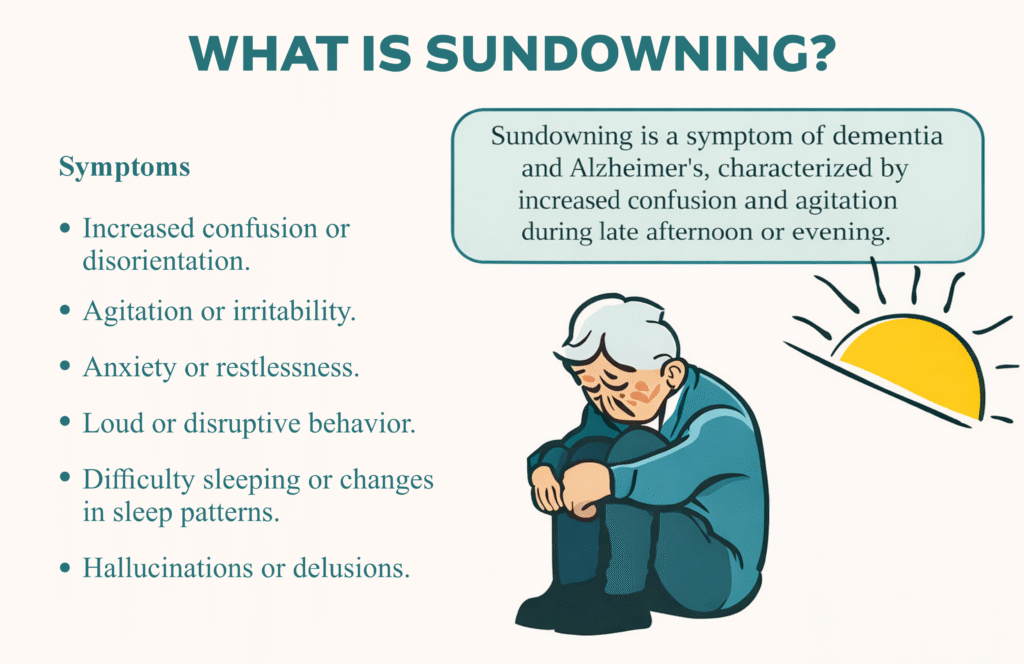
What Is Sundowning in Dementia and Why It Happens
Sundowning in dementia is a pattern of increased confusion, agitation, and behavioral changes that appear later in the day, typically as daylight fades. It is not a disease on its own; it is a symptom seen in people living with conditions like Alzheimer’s or vascular dementia. Many caregivers also hear it described as “sundowner syndrome,” which reflects the same late-day changes.
You may notice that a calm loved one suddenly becomes restless, anxious, or even upset without a clear reason. In some cases, dementia and being mean to family can become more noticeable during these hours, not because the person intends harm, but because their brain struggles to process reality, emotions, and surroundings.
Why does sundowning happen?
Sundowning happens due to a combination of physical and environmental factors:
- Brain changes from dementia disrupt the body’s internal clock (circadian rhythm)
- Fatigue builds up after a full day of activity
- Reduced daylight and increasing shadows (sometimes called night shading) create confusion
- Difficulty distinguishing reality from imagination may lead to fear or suspicion
In some cases, these changes can lead to aggressive dementia behaviors, including shouting, pacing, or resisting care. This can feel overwhelming for caregivers, especially when it happens suddenly or daily.
Understanding what is sundowning in dementia helps you recognize that these behaviors are not personal, they are part of how the condition affects the brain.
RELATED: Will a Bladder Infection Cause Nausea UTI? A Caregiver’s Guide (2026)
What Time Does Sundowning Start, and How Long Does It Last?
Sundowning usually begins in the late afternoon, around 3 p.m. to 5 p.m., and can continue into the evening and night. For many caregivers, the timing closely follows sunset, so checking what time is sundown today or what time is sundown tonight can help you anticipate when symptoms may begin.
When does it peak?
Symptoms often peak around sunset, when natural light fades, and shadows increase. During this period, you may notice:
- Increased confusion
- Restlessness or pacing
- Anxiety or irritability
How long does sundowning last?
Sundowning can last for several hours, sometimes easing once the person settles into nighttime routines or sleep. However, the duration varies:
- Some individuals calm down after a few hours
- Others may remain unsettled late into the night
Does it always happen in the evening?
Not always. While evening is most common:
- Some people experience sundowning in the morning, especially if their sleep cycle is disrupted
- Others may have irregular patterns depending on fatigue, environment, or health changes
Is sundowning linked to life expectancy?
Many caregivers ask about life expectancy with sundowners, but sundowning itself does not determine lifespan. It reflects how dementia affects brain function and daily rhythms, not how long someone will live.
Understanding what time is sundowning allows you to prepare ahead, adjust lighting, reduce stimulation, and create a calm routine before symptoms escalate.
What Triggers Sundowning in Dementia Patients?
Sundowning does not happen randomly. Certain factors increase confusion and agitation, especially later in the day. When caregivers understand what triggers sundowning, they can prevent or reduce many episodes before they escalate.
Common triggers of sundowning
- Fatigue after a long day
The brain becomes more overwhelmed as energy levels drop.
- Low lighting and shadows (night shading)
Dim environments can distort perception and increase fear or confusion.
- Disrupted body clock (circadian rhythm)
Dementia affects the brain’s ability to regulate sleep and wake cycles.
- Hunger, dehydration, or discomfort
Unmet physical needs can quickly turn into agitation.
- Unfamiliar environments or changes in routine
New settings or unexpected changes can increase anxiety.
- Medications that cause sundowning
Some drugs, especially sedatives or medications affecting sleep, may worsen confusion or agitation.
- Underlying medical issues
Infections, pain, or conditions like urinary tract infections can intensify symptoms.
Does the type of dementia matter?
Yes. For example, vascular dementia sundowning may present differently depending on how blood flow changes affect the brain. Some individuals may experience more sudden mood shifts or confusion compared to other types of dementia.
Caregiver insight
You may notice patterns over time. For example:
- Agitation increases after poor sleep
- Confusion worsens in dim lighting
- Behavior changes after certain medications
Tracking these patterns helps you identify what triggers sundowning for your loved one specifically, and respond more effectively.
READ MORE: What is an SR1 Form? 2026 Guide for UK Care Providers
Is Sundowning a Sign of Death or Disease Progression?
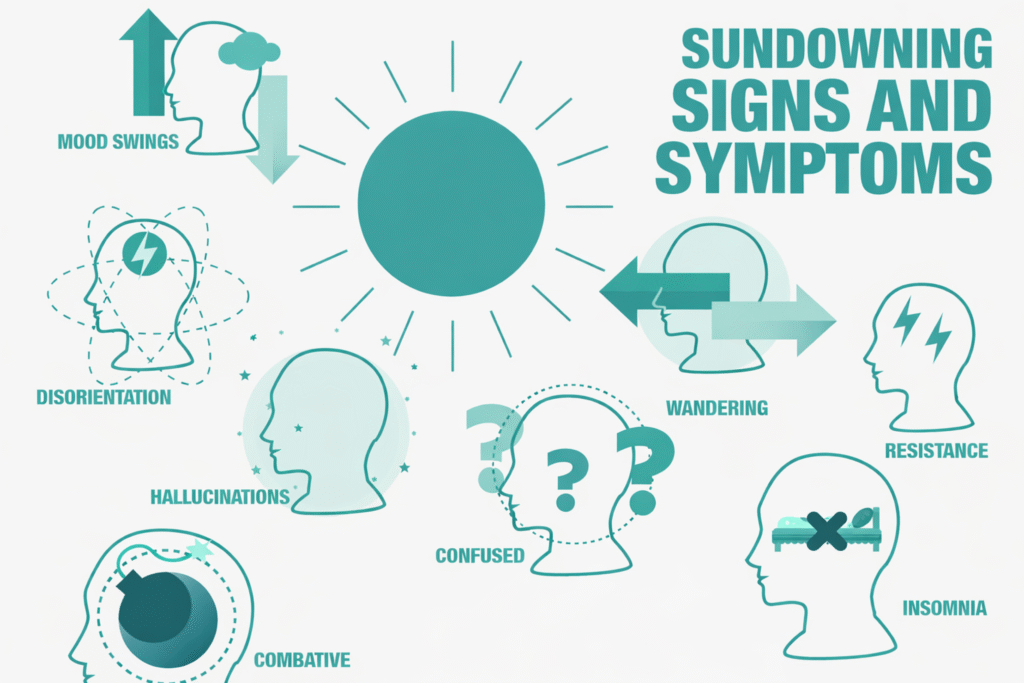
No, sundowning is not a sign of death. It does not mean that a person is nearing the end of life. Instead, sundowning reflects how dementia affects the brain’s ability to regulate behavior, light perception, and daily rhythms.
What sundowning actually indicates
Sundowning usually signals:
- Changes in brain function caused by dementia
- Increased sensitivity to fatigue and environmental changes
- Disruption in the body’s internal clock (sleep–wake cycle)
As dementia progresses, these symptoms may become more noticeable, but they do not directly predict how long someone will live.
Understanding the confusion around life expectancy
Many caregivers search for life expectancy with sundowners, but it’s important to separate the two:
- Sundowning is a behavioral pattern, not a disease stage
- Life expectancy depends on the type and progression of dementia, overall health, and care quality
- Some individuals experience sundowning early, while others develop it later
When should you be concerned?
While sundowning itself is not a sign of death, you should seek medical advice if:
- Symptoms suddenly worsen
- Behavior changes become extreme or unsafe
- There are signs of infection, pain, or medication side effects
In some cases, medications that cause sundowning or untreated health issues can make symptoms appear more severe than they actually are.
Caregiver reassurance
It can feel alarming when a loved one becomes confused or agitated every evening. However, understanding that sundowning is a manageable symptom, not a terminal signal, helps you respond with clarity and confidence.
SEE ALSO: What is the Health and Safety at Work Act 1974?
Can Sundowning Occur Without Dementia?

Yes, sundowning without dementia can happen, but it is less common. In most cases, sundowning is strongly linked to dementia, especially Alzheimer’s disease. However, similar late-day confusion or agitation can appear in people without a formal dementia diagnosis.
When sundowning happens without dementia
You may notice sundowning-like symptoms in situations such as:
- Delirium (sudden confusion)
Often caused by infections, medication changes, or hospitalization
- Severe sleep disruption
Poor sleep can confuse the brain’s internal clock and mimic sundowning patterns
- Stress or anxiety
Emotional strain can increase restlessness or irritability later in the day
- Medication side effects
Some medications that cause sundowning, such as sedatives or drugs affecting the nervous system, can trigger confusion even without dementia
How to tell the difference
- Dementia-related sundowning tends to be consistent and progressive
- Non-dementia cases are often sudden and reversible once the underlying cause is treated
For example, if confusion appears quickly and worsens over a few days, a medical issue like an infection may be the cause, not dementia.
Caregiver guidance
If you notice sundowning behaviors in someone without a dementia diagnosis:
- Seek medical evaluation promptly
- Review recent medication changes
- Monitor sleep patterns and daily routines
Understanding whether symptoms are due to sundowning dementia or another condition helps you take the right action early.
MORE: How Much Is JSA (Jobseeker’s Allowance) in 2026?
How to Deal With Aggressive Dementia and Sundowning Behaviour
Sundowning can sometimes lead to aggressive dementia behaviors, including shouting, resistance to care, or even physical actions. As a caregiver, these moments can feel overwhelming, but your response can either calm or escalate the situation.
Why aggression happens during sundowning
Aggression often comes from:
- Fear and confusion as surroundings become harder to recognize
- Frustration from not being understood
- Overstimulation or fatigue late in the day
- Misinterpretation of people or shadows (especially with low lighting)
In many cases, what looks like anger is actually distress.
What to do with a violent dementia patient
If behavior becomes intense or unsafe:
- Stay calm and keep your voice steady
Your tone directly affects their reaction
- Give space and avoid confrontation
Do not try to physically restrain unless absolutely necessary
- Redirect attention
Shift focus to a calming activity like music or a familiar object
- Remove triggers
Reduce noise, dim harsh lighting, and create a quiet environment
- Ensure safety first
Move sharp objects away and position yourself safely
How to deal with dementia patients who is aggressive
Use these daily strategies to reduce escalation:
- Keep a consistent routine
Predictability reduces anxiety
- Use simple, clear communication
Avoid long explanations or arguments
- Validate their feelings
Instead of correcting them, respond with reassurance
- Watch for patterns
Identify what triggers sundowning and act early
- Stay patient, even when it’s difficult
Remember, the behavior is caused by the condition—not intent
Caregiver reality
Many caregivers struggle with dementia and being mean to family, especially during sundowning hours. It can feel personal, but it isn’t. The brain can no longer process emotions and reality correctly, which leads to reactions that seem out of character.
Understanding this helps you respond with empathy instead of frustration, and that alone can reduce how often aggressive episodes occur.
READ: What Is an Enhanced DBS CRB Check? 2026 Update for Care Homes
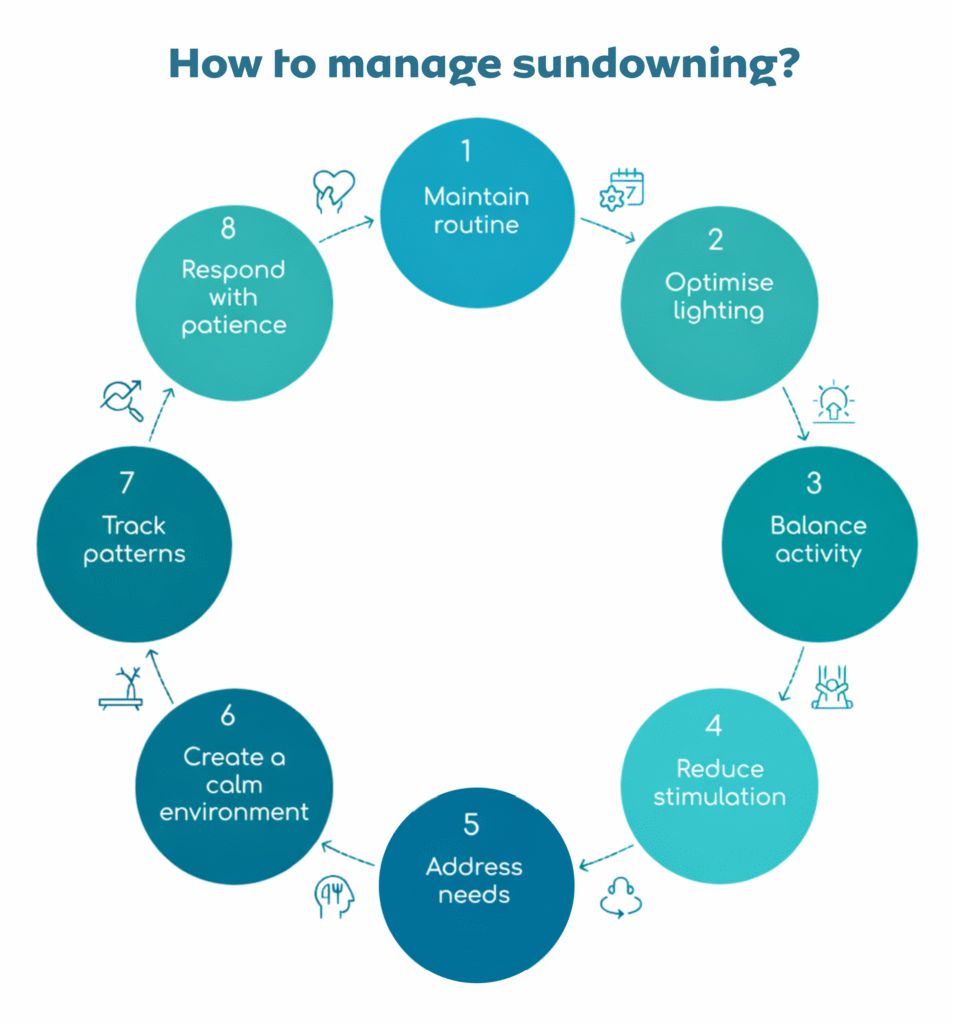
How Caregivers Can Reduce Sundowning Symptoms
You cannot completely eliminate sundowning, but you can reduce how often it happens and how intense it becomes. Small changes in routine and environment make a big difference, especially when you apply them before symptoms start.
Create a calm, predictable routine
- Keep consistent times for waking, meals, and bedtime
- Schedule demanding activities earlier in the day
- Avoid sudden changes in routine
A stable routine helps regulate the brain and reduces confusion later in the day.
Manage light and environment
- Turn on lights before it gets dark to reduce shadows (night shading)
- Keep rooms well-lit and familiar
- Reduce background noise (TV, loud conversations)
Matching your environment to what time is sundown today UK can help you act early, before agitation begins.
Reduce physical and mental triggers
- Offer meals and fluids regularly to avoid hunger or dehydration
- Limit caffeine, especially in the afternoon
- Encourage short rest periods, but avoid long daytime naps
Also review any medications that cause sundowning, especially if symptoms suddenly worsen.
Use calming activities
- Play familiar, gentle music
- Look through family photos
- Take a short walk during daylight hours
These activities help shift focus and reduce anxiety.
Monitor patterns and act early
Track:
- When symptoms start (based on what time is sundowning)
- What happened earlier in the day
- Environmental changes (lighting, noise, visitors)
Over time, you’ll identify patterns and prevent triggers before they escalate.
Caregiver reminder
Sundowning can be exhausting, especially when it happens daily. But early preparation, calm responses, and small adjustments can significantly reduce stress for both you and your loved one.
Final Thoughts…
Sundowning can feel unpredictable and exhausting, especially when behavior changes happen at the same time every day. But once you understand what time is sundowning and what drives it, you gain something powerful, control through preparation.
You are not dealing with intentional behavior. You are responding to how dementia changes the brain’s ability to process light, time, and surroundings. That’s why simple steps, like adjusting lighting, maintaining routines, and staying calm, can make a meaningful difference.
Focus on what you can control:
- Prepare before late afternoon
- Reduce known triggers
- Respond with patience, not confrontation
Over time, you will begin to recognize patterns, anticipate changes, and handle even difficult moments, like aggressive dementia behaviors, with more confidence.
Most importantly, take care of yourself too. Supporting someone with sundowning dementia is demanding, and your well-being matters just as much as theirs.
Need Support Managing Sundowning in Your Care Service?
Sundowning can quickly lead to distress, aggression, and unsafe situations if not managed early.
Care Sync Experts helps you:
- Reduce agitation and aggressive dementia episodes
- Train staff to handle difficult behaviours confidently
- Build structured routines that prevent escalation
- Stay compliant with care standards
Book a Free Care Support Consultation
Get practical, expert guidance to improve care outcomes and reduce daily stress for your team.
FAQ
Why is sundowning worse at night?
Sundowning becomes worse at night because the brain struggles more with fatigue, low lighting, and disrupted internal rhythms. As daylight fades, shadows increase and visibility drops, which can confuse a person with dementia. Combined with a full day of mental activity, this often leads to heightened agitation, anxiety, and disorientation in the evening.
Can sundowning happen after midnight?
Yes, sundowning can continue after midnight, especially if the person has not settled or has disrupted sleep. While symptoms usually begin in the late afternoon, some individuals remain restless, confused, or awake throughout the night. Poor sleep patterns can extend or worsen these behaviors.
What is the morning version of sundowning?
Some caregivers notice similar symptoms earlier in the day, often called “morning confusion” or reversed sundowning.” This can happen when sleep cycles are severely disrupted. Instead of worsening in the evening, the person may wake up confused, agitated, or disoriented in the morning.
How to respond to sundowning?
Responding effectively requires calm, proactive care:
– Stay calm and speak in a reassuring tone
– Avoid arguing or correcting the person
– Redirect attention to a calming activity
– Keep the environment quiet and well-lit
– Maintain a consistent routine
The goal is not to “fix” the behavior instantly, but to reduce distress and create a sense of safety for the person.
