Part L building regulations are UK rules that set minimum energy efficiency standards for buildings, including how they are designed, heated, insulated, and ventilated. In England, these requirements are explained in Approved Document L, which applies to both new buildings and existing properties undergoing renovation or extension.
For care businesses, Part L UK matters whenever you build, convert, extend, or upgrade a property. Whether you are opening a new care home, converting a house into supported living, or improving an office space, you must meet Part L compliance standards before the building can be approved for use.
The latest updates, often referred to as Part L building regulations 2022, came into effect on 15 June 2022 under the Part L building regulations 2021 framework (with later amendments). These changes introduced stricter requirements to reduce energy use and carbon emissions, as part of the UK’s wider push toward net zero.
In simple terms, building regs Part L ensure that:
- Buildings lose less heat through walls, roofs, and windows
- Heating systems run efficiently and use less energy
- Ventilation systems maintain air quality without wasting heat
- Developers and contractors provide clear evidence that work meets required standards
For care providers, this is not just a technical requirement. It directly affects:
- resident comfort and safety
- energy costs and long-term operating expenses
- whether a building can legally open or continue operating
Understanding Part L building regulations early helps care businesses avoid delays, reduce costs, and make smarter decisions when planning or upgrading their services.

Why care businesses should pay attention to Part L
Care businesses cannot treat Part L building regulations as a “builder’s problem.” These rules directly affect how you open, run, and scale your service.
Energy efficiency is not just about compliance; it shapes your daily operations.
1. It directly impacts your running costs
Care homes and supported living services operate 24/7. Heating, hot water, and ventilation run constantly.
Poor Part L compliance means:
- higher energy bills
- inefficient heating systems
- long-term financial pressure
Meeting building regs Part L standards helps you reduce energy waste and protect your margins.
2. It affects resident comfort and care quality
Warm, well-ventilated environments are essential in care settings.
Strong insulation and proper Part L building Regulations ventilation improve:
- indoor temperature stability
- air quality for vulnerable residents
- infection control and overall wellbeing
If you get this wrong, you don’t just fail compliance, you compromise care standards.
3. It determines whether your project can open on time
If your building fails Part L UK requirements, building control can delay or block approval.
This can lead to:
- delayed service launch
- lost revenue
- costly redesigns or rework
Many care providers only discover issues late, when fixes become expensive and disruptive.
4. It influences funding, inspections, and reputation
Energy-efficient buildings increasingly align with:
- investor expectations
- local authority commissioning standards
- sustainability requirements
A care provider that meets Part L building regulations 2022 standards positions itself as:
- modern
- compliant
- future-ready
5. It affects every type of care setup
Whether you run:
- a care home
- supported living accommodation
- domiciliary care offices
Part L building regulations still apply when you:
- refurbish
- extend
- convert buildings
- upgrade heating or insulation
Part L is not just a construction rule; it is a business decision.
Care providers who understand it early:
- avoid delays
- control costs
- deliver better environments for residents
Those who ignore it often pay for it later, financially and operationally.
RELATED: What Is the Care Certificate? 2026 Update
What does Part L actually cover?
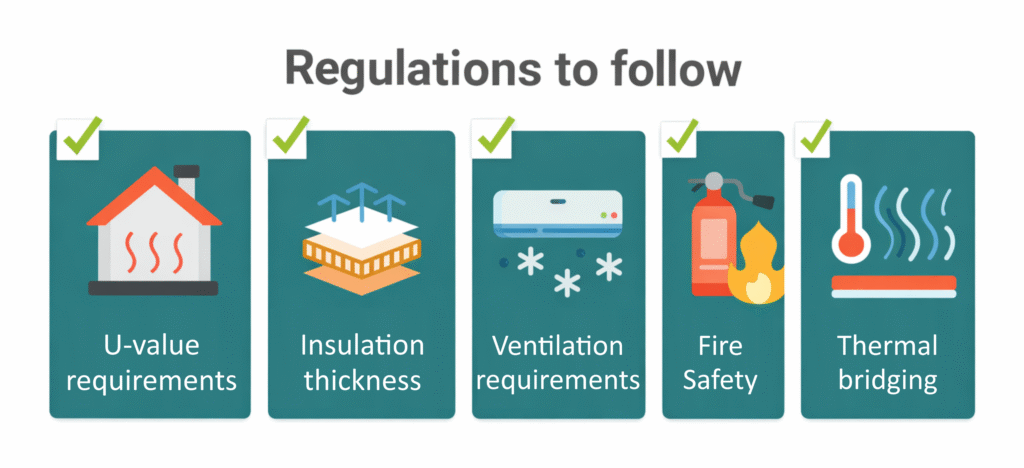
Part L building regulations focus on how a building uses energy and how much heat it loses. In England, Approved Document L explains how to meet these requirements in practice.
For care businesses, this section answers a simple question: What exactly do we need to get right before a building is approved?
1. Two main categories: dwellings vs non-dwellings
Part L UK splits buildings into two groups:
- Dwellings (Part L1A / L1B)
Homes where people live independently (e.g. some supported living setups)
- Non-dwellings (Part L2A / L2B)
Commercial or institutional spaces (e.g. care homes, offices, clinics)
Most care homes fall under Part L building regulations non dwellings, while supported living can fall under either category depending on layout and level of independence.
Getting this classification wrong can lead to incorrect design, failed approval, and delays.
2. Fabric performance (how well the building retains heat)
Building regs Part L require strong insulation across:
- walls
- roofs
- floors
- windows and doors
This is measured using U-values (how much heat escapes).
For care providers, this means:
- better temperature control for residents
- reduced heating demand
- lower long-term costs
3. Heating and hot water systems
Part L building regulations push for more efficient, low-carbon systems.
This includes:
- modern boilers or heat pumps
- lower flow temperatures
- smarter controls
For care environments, heating must balance:
- energy efficiency
- consistent warmth for vulnerable residents
4. Ventilation and air quality
Part L building Regulations ventilation works alongside other rules to ensure buildings stay healthy as they become more airtight.
This includes:
- mechanical or natural ventilation systems
- controlled airflow
- reduced heat loss while maintaining fresh air
This is critical in care settings, where air quality directly affects health outcomes.
5. Energy modelling and calculations
To prove compliance, developers must use:
- SAP (for dwellings)
- SBEM (for non-dwellings)
These models calculate:
- energy use
- carbon emissions
- overall efficiency
Care businesses don’t need to run these models, but you must ensure your project team does.
6. Evidence and documentation
One of the biggest changes under Part L building regulations 2022 is stricter proof requirements.
You must provide:
- design-stage calculations
- as-built performance reports
- photographic evidence of construction details
Without this, you cannot demonstrate Part L compliance, even if the building is physically correct.
Approved Document L is not just guidance, it defines what your building must achieve to pass.
For care providers, it covers:
- how your building is built
- how it performs
- how you prove it meets the rules
Understanding this early helps you avoid costly mistakes and ensures your project meets Part L building regulations from day one.
READ MORE: What are Cold Weather Payments? Eligibility & How to Claim (2026)
Which care projects does Part L affect most?
Many care providers assume Part L building regulations only apply to large construction projects. In reality, they affect almost every type of property change in the care sector.
If you run or plan to expand a care business, you will likely trigger Part L compliance at some point.
1. Opening a new care home
New-build care homes fall fully under building regs Part L, usually within the Part L building regulations non dwellings category.
You must meet strict requirements for:
- insulation and airtightness
- heating system efficiency
- ventilation design
- full energy modelling and evidence
These projects must align with Part L building regulations 2022, which introduced tighter carbon reduction targets.
2. Converting buildings into supported living
Conversions are common in the care sector, but they come with risk.
If you convert:
- a house into supported living
- a commercial building into a care facility
You must meet Part L building regulations 2021 standards for existing buildings.
This often means:
- upgrading insulation
- improving heating systems
- meeting minimum energy performance levels
Many providers underestimate how much upgrade work is required.
3. Extending an existing care home
Adding new rooms, wings, or facilities triggers Part L UK requirements.
You must ensure:
- the new extension meets current energy standards
- the connection between old and new parts does not create heat loss issues
Even small extensions can require significant upgrades to meet compliance.
4. Refurbishing or upgrading existing buildings
Even if you are not building new, Part L building regulations still apply when you:
- replace windows or doors
- upgrade insulation
- install a new heating system
- carry out major renovation work
These fall under Part L1B or L2B, depending on the building type.
Many care providers trigger compliance without realising it.
5. Setting up or upgrading a domiciliary care office
Office spaces may seem simple, but they still fall under building regs Part L.
If you:
- move into a new office
- refit an existing one
- upgrade heating or ventilation
You may need to meet energy efficiency standards and provide compliance evidence.
6. Special cases and older buildings
Some care providers operate in older or unique properties, such as a grade 2 listed building.
In these cases:
- full compliance may not always be possible
- adjustments or alternative approaches may apply
However, you should never assume exemption without expert advice under Part L building Regulations exemptions.
SEE ALSO: Does Cold Weather Make You Sick? The Complete 2026 Guide
Part L Requirements Care Providers Should Understand Before Starting Work
Before you start any project, you need a clear understanding of what Part L building regulations actually require in practice. This is where many care businesses make costly mistakes, by relying entirely on contractors without understanding the basics.
1. Insulation and building fabric
Building regs Part L place strong emphasis on how well your building retains heat.
You must ensure:
- walls, roofs, and floors meet minimum insulation standards
- windows and doors limit heat loss
- gaps and air leakage are controlled
Better insulation means:
- more stable indoor temperatures
- improved comfort for residents
- lower energy bills over time
2. Heating and hot water systems
Part L building regulations 2022 push for more efficient and lower-carbon systems.
Your project must include:
- energy-efficient boilers or heat pumps
- properly sized systems for the building
- modern controls to manage temperature effectively
In care settings, you must balance efficiency with reliability, residents cannot tolerate inconsistent heating.
3. Ventilation and air quality
As buildings become more airtight, ventilation becomes critical.
Part L building Regulations ventilation ensures:
- fresh air circulation
- removal of moisture and pollutants
- reduced risk of overheating
This often includes:
- mechanical ventilation systems
- heat recovery systems in some cases
Poor ventilation can lead to:
- damp and mould
- poor air quality
- increased health risks for residents
4. Energy modelling and performance targets
To prove Part L compliance, your project team must complete energy calculations.
These include:
- SAP for dwellings
- SBEM for non-dwellings
These models assess:
- carbon emissions
- energy consumption
- overall building performance
You don’t need to run these models yourself, but you must ensure they are completed correctly.
5. Evidence and documentation (often overlooked)
One of the biggest shifts in Part L UK is the requirement to prove compliance, not just claim it.
You must provide:
- design-stage energy reports
- as-built performance reports
- photographic evidence of key construction stages
Photos must clearly show:
- insulation installation
- junction details where heat loss can occur
- key building elements before they are covered
Without proper evidence, your building may fail approval, even if the work is correct.
6. Responsibility and coordination
Many care providers assume the builder handles everything.
In reality:
- contractors build
- consultants calculate
- building control verifies
- you remain responsible as the client
You must ensure:
- the right professionals are involved early
- compliance is considered from design stage
- documentation is properly managed
MORE: Children’s DLA Rates: Who Qualifies, and What to Claim in 2026
How Part L Links with Other Rules Care Businesses May Hear About

When you plan a care project, you will hear multiple regulations, not just Part L building regulations. This can feel overwhelming, especially if you are not from a construction background.
The key is to understand what each rule covers and how they connect.
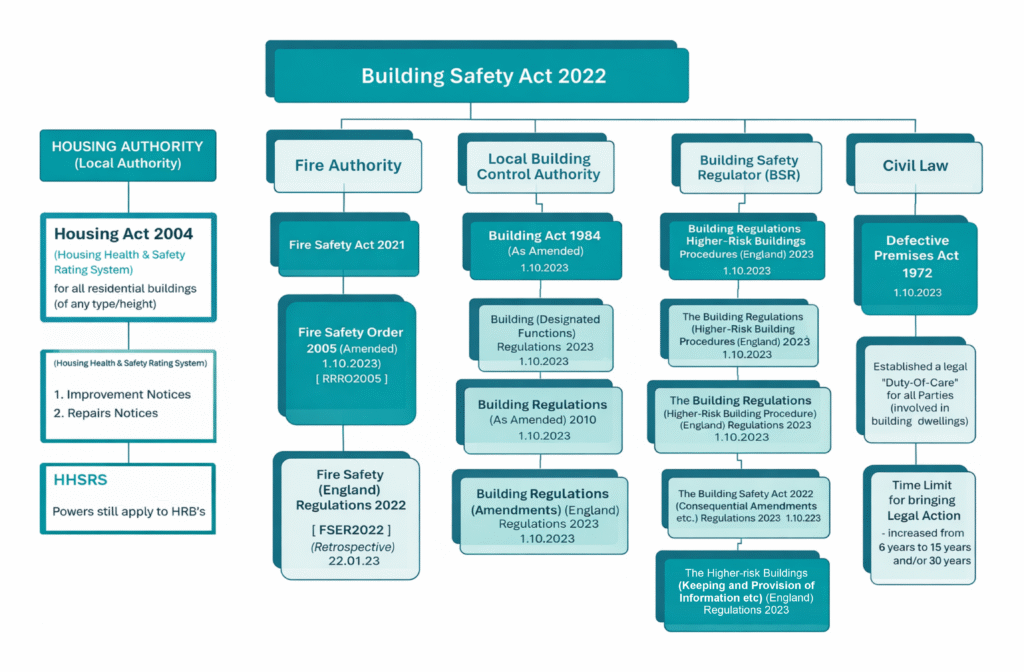
1. Part L vs the Building Safety Act
Part L focuses on energy efficiency. The Building Safety Act and building safety act 2022 focus on safety, accountability, and documentation.
For care providers, this means:
- Part L ensures your building performs efficiently
- The Building Safety Act ensures your building is safe and properly documented
Both require strong record-keeping and evidence, especially for larger or higher-risk buildings.
2. Part L vs Part M (accessibility)
You will often hear about part m building regulations or approved document m during care projects.
- Part L = energy efficiency
- Part M = accessibility and usability
In care settings, building regs part m is critical because it covers:
- wheelchair access
- bathroom layouts
- safe movement within the building
You must meet both standards at the same time; one does not replace the other.
3. Part L vs fire safety rules (Part B)
Fire safety falls under:
- approved doc b
- building regs part b
These rules focus on:
- fire detection systems
- escape routes
- compartmentation
While Part L UK focuses on insulation and airtightness, you must ensure these do not conflict with fire safety design.
4. Other related regulations you may encounter
Depending on your project, you may also hear about:
- approved document k (safety around stairs, ramps, and movement)
- general building regulations covering structure and ventilation
These do not replace Part L building regulations, but they run alongside them.
5. Why this matters for care providers
Care projects rarely deal with one regulation in isolation.
If you:
- build a new care home
- convert a property
- extend an existing facility
You will need to meet multiple standards at once.
The biggest risk is:
- focusing on energy efficiency
- while overlooking access, safety, or usability
Part L building regulations form just one part of a wider compliance framework.
For care providers:
- Part L = energy performance
- Part M = accessibility
- Part B = fire safety
- Building Safety Act = accountability and safety systems
Understanding how they work together helps you:
- avoid design conflicts
- prevent costly redesigns
- ensure your building meets all approval requirements the first time
SEE: Equality Act Protected Characteristics: 2026 Importance for Care Work
Are there any exemptions or special cases under Part L?

Many care providers ask whether Part L building regulations always apply in full. The answer is: not always, but exemptions are limited and highly controlled.
You should never assume you qualify for Part L building Regulations exemptions without proper advice.
1. Existing and older buildings
When you upgrade an existing property, Part L allows some flexibility.
For example:
- you may not need to upgrade every element to new-build standards
- improvements must be “reasonable and practical”
However, you still need to:
- improve energy performance where possible
- avoid making the building worse
Even partial refurbishment can still trigger Part L compliance requirements.
2. Listed and heritage buildings
Care providers sometimes operate in older or historic properties, such as a grade 2 listed building.
In these cases:
- strict upgrades (like replacing windows or external insulation) may not be allowed
- heritage protection can limit what changes you can make
However:
- you must still improve energy efficiency where it does not damage the building’s character
This often requires:
- specialist advice
- tailored solutions
3. Technical and practical limitations
Some buildings cannot meet full modern standards due to:
- structural limitations
- space constraints
- compatibility with existing systems
In these situations:
- alternative measures may be accepted
- compliance focuses on “reasonable improvement” rather than perfection
4. What does NOT count as an exemption
Care providers often misunderstand this.
You are not exempt just because:
- the building is old
- the project is small
- you are only making minor changes
- you are leasing the property
If your work affects energy performance, building regs Part L will likely apply.
5. Why exemptions still require documentation
Even when flexibility applies, you must:
- justify your approach
- document decisions
- show why full compliance was not possible
Building control will still expect:
- clear reasoning
- supporting evidence
Part L building regulations rarely offer full exemptions.
In most cases:
- you must comply fully
- or improve performance as far as reasonably possible
Care providers who assume they are exempt often face:
- delays
- redesign costs
- compliance issues during approval
The safest approach is simple:
Always check early, plan properly, and treat Part L compliance as part of your core project strategy.
LEARN MORE: How to Choose Home Care Agencies in the UK (2026)
Common mistakes care businesses make with Part L

Many care providers run into problems with Part L building regulations, not because the rules are unclear, but because they get involved too late or rely on the wrong assumptions.
Avoiding these mistakes can save you time, money, and project delays.
1. Treating Part L as the builder’s responsibility
Many providers assume the contractor will “handle compliance.”
In reality:
- you own the project
- you remain responsible for Part L compliance
- poor coordination can still lead to failure
You need visibility from design to completion.
2. Signing a lease or buying a property without checking requirements
This is one of the most expensive mistakes.
Care providers often:
- secure a building first
- check building regs Part L later
This can lead to:
- unexpected upgrade costs
- delays in opening
- redesign of heating, insulation, or ventilation systems
Always assess Part L building regulations before committing to a property.
3. Assuming only new builds are affected
Many providers think Part L UK only applies to new construction.
In reality, it also applies when you:
- refurbish
- extend
- replace key building elements
Even simple upgrades can trigger compliance requirements.
4. Ignoring ventilation when improving insulation
Improving insulation without considering Part L building Regulations ventilation creates serious problems.
This can lead to:
- poor air quality
- damp and mould
- overheating
Energy efficiency must always balance with ventilation.
5. Underestimating documentation and evidence
Some providers focus on the physical build but forget about proof.
Under Part L building regulations 2022, you must provide:
- energy calculations
- as-built reports
- photographic evidence
Without this, your project may fail, even if everything is installed correctly.
6. Leaving compliance too late in the project
If you only think about Part L during construction, you are already at risk.
Late changes can mean:
- redesigning systems
- replacing materials
- increased costs
The best projects consider compliance at the design stage.
7. Not involving the right professionals early
Successful projects require:
- energy assessors
- consultants
- experienced contractors
If you delay bringing them in:
- mistakes go unnoticed
- compliance gaps increase
Bottom line
Most Part L building regulations issues come down to timing and awareness.
Care providers who:
- plan early
- ask the right questions
- stay involved
Avoid delays, reduce costs, and achieve smooth approvals.
Those who don’t often face:
- rework
- compliance failures
- delayed service launches
Final takeaway for care providers
Part L building regulations are not just a technical requirement, they directly shape how your care business operates, grows, and delivers safe environments.
If you plan to:
- open a new service
- convert a property
- extend or refurbish a building
You must consider Part L compliance from the very beginning.
Care providers who approach Part L UK correctly:
- control energy costs
- create comfortable, healthy environments for residents
- avoid delays during approval
- protect their investment
Those who ignore it often face:
- unexpected upgrade costs
- failed inspections
- delayed openings
The simple rule to follow
Treat building regs Part L as a business priority, not just a construction detail.
If you:
- check requirements early
- work with the right professionals
- plan for both performance and evidence
You will meet compliance smoothly and avoid costly mistakes.
One final perspective
Energy efficiency is no longer optional. It sits at the centre of modern care delivery.
Understanding Part L building regulations helps you:
- build smarter
- operate more efficiently
- deliver better care environments
And in a sector where comfort, safety, and sustainability matter every day…
That is a competitive advantage.
Need Expert Support Navigating Building Compliance and Care Facility Requirements?
Care Sync Experts supports care providers, care home operators, and healthcare organisations across the UK with clear, practical guidance on regulatory compliance, property requirements, and operational readiness.
From helping you understand Part L building regulations, energy efficiency standards, and building compliance requirements, to guiding you through property conversions, refurbishments, and service setup, our specialists turn complex regulations into simple, actionable steps.
Whether you are opening a new care home, converting a property into supported living, upgrading your facilities, or ensuring full Part L compliance alongside CQC expectations, our team delivers tailored support designed for real-world care environments.
Plan smarter, avoid costly mistakes, and ensure your care premises meet all regulatory standards from day one.
Contact Care Sync Experts today to get expert support on building compliance, care facility setup, and navigating UK care regulations with confidence.
FAQ
Is Part L law in the UK?
Yes. Part L building regulations form part of the Building Regulations in England and are legally enforceable. While Approved Document L provides guidance on how to meet the requirements, the underlying regulation itself is law.
If a care provider or developer fails to meet Part L compliance, building control can:
– refuse approval
– require corrective work
– issue fines or enforcement action
In simple terms: you must comply with Part L to legally complete and use a building.
What are carbon emission targets in Part L?
Part L building regulations 2022 introduced stricter carbon reduction targets as part of the UK’s journey toward net zero.
For new buildings:
– new homes must reduce carbon emissions by around 30% compared to previous standards
– future standards aim for 75–80% reductions by 2025
For care providers, this means:
– more efficient heating systems
– better insulation
– lower overall energy use
These targets directly influence design, costs, and long-term energy performance.
What is the 10 year rule for listed buildings?
The “10-year rule” is often misunderstood. It does not automatically exempt buildings from regulation, including Part L building regulations.
In planning terms, it generally refers to situations where:
– unauthorised work may become lawful after 10 years if no enforcement action is taken
However, for buildings such as a grade 2 listed building:
– separate listed building consent rules still apply
– energy upgrades must balance compliance with heritage protection
Care providers should always seek professional advice; never assume older or listed buildings are exempt from compliance requirements.
What are the 7 stages of construction?
Understanding the construction process helps care providers manage Part L compliance effectively.
The typical stages are:
– Planning and feasibility
– Design and approvals
– Procurement and contractor selection
– Site preparation
– Construction
– Inspection and compliance checks
– Completion and handover
Part L building regulations apply across multiple stages, especially:
– design (energy modelling and specifications)
– construction (installation quality)
– completion (evidence and certification)
Getting involved early in these stages helps care businesses avoid delays and ensure smooth approval.