Person centred care is an approach to healthcare and social care that places the individual receiving care at the centre of all decisions about their support, treatment, and wellbeing. Instead of focusing only on a condition or illness, professionals consider the person’s preferences, values, lifestyle, and goals when delivering care.
In simple terms, the person centred care meaning is providing care that respects the whole person and involves them as an active partner in decisions about their health.
When people ask what is person centred care, the answer often overlaps with patient centred care and the person centred approach used across health and social care services. Caregivers, nurses, and support staff work collaboratively with individuals and their families to design care that fits their needs. This approach ensures that care remains respectful, personalised, and responsive rather than standardised or task-focused.
In practice, person centred care in health and social care means listening carefully to the individual, adapting care plans to reflect their wishes, and supporting them to maintain independence whenever possible. Care providers move beyond simply treating symptoms and instead focus on improving the person’s overall quality of life, dignity, and wellbeing.

What Is Person-Centred Care in Health and Social Care?
In care in health and social care, a person centred approach means caregivers design support around the individual rather than around routines, institutions, or medical conditions. Care professionals listen to the person, understand their preferences, and adapt services to support their physical, emotional, and social needs.
For example, a domiciliary caregiver visiting someone at home does more than complete scheduled tasks. They ask about the person’s daily routine, preferred meals, cultural practices, and personal goals. The caregiver then adjusts care plans so the support reflects the individual’s lifestyle rather than forcing the person to adapt to a rigid service structure.
In hospitals, nursing teams use person centred care by involving patients in treatment decisions and clearly explaining available options. In care homes, resident site staff encourage residents to maintain independence, make choices about their day, and participate in activities that matter to them.
Ultimately, what is person-centred care in health and social care comes down to one principle: treating people as individuals with unique lives, experiences, and priorities. When caregivers adopt this mindset, care becomes more respectful, more effective, and far more meaningful for the person receiving support.
RELATED: What Is a Care Needs Assessment? (England Guide for Families and Caregivers)
What Are the 4 Principles of Person-Centred Care?
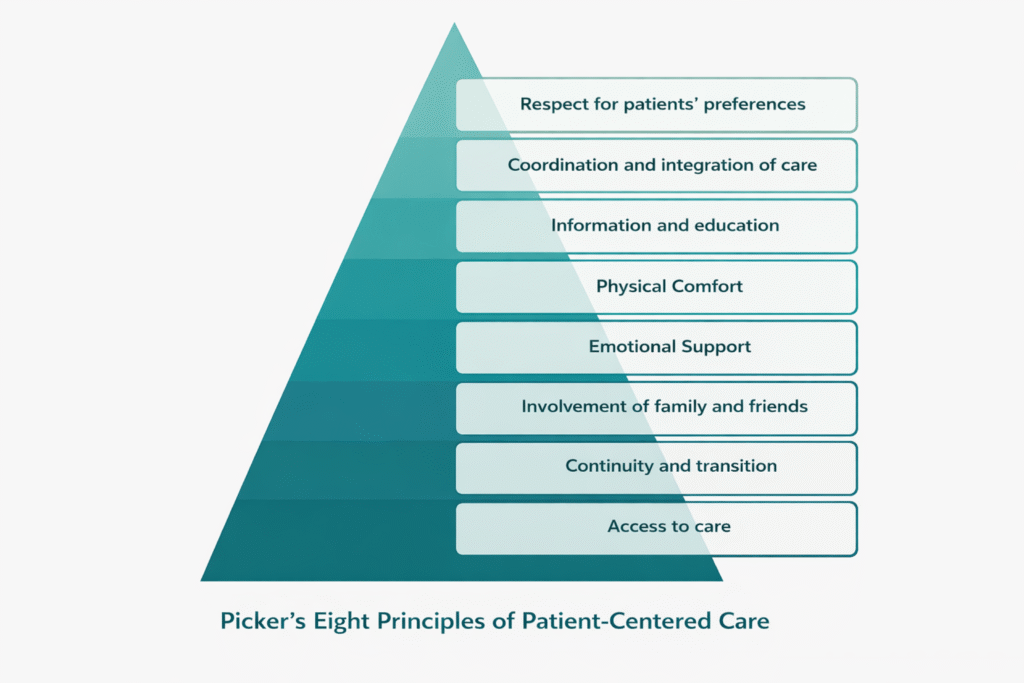
To understand what are the 4 principles of person-centred care, caregivers should focus on four core ideas that guide how support is delivered in care in health and social care settings. These principles ensure that person centred care remains respectful, collaborative, and responsive to individual needs.
1. Respect and Dignity
Care providers must treat every individual with dignity, compassion, and respect. This means recognising personal beliefs, cultural values, and privacy needs. Caregivers should listen carefully, avoid assumptions, and ensure that each person feels valued and heard.
2. Individualised Care
No two people have the same needs. A person centred approach requires caregivers to tailor care plans around the individual’s health condition, daily routine, preferences, and long-term goals. Support should adapt to the person rather than forcing the person to adapt to the service.
3. Shared Decision-Making
Person centred care encourages individuals to take an active role in decisions about their treatment and support. Care professionals provide clear information about options and work with the person to decide what approach best suits their circumstances.
4. Independence and Empowerment
Care should help individuals maintain control over their lives whenever possible. Caregivers support people to build confidence, make informed choices, and manage aspects of their own health and wellbeing. Empowerment helps improve both outcomes and quality of life.
Together, these four principles form the foundation of person centred care, guiding caregivers to deliver support that respects the whole person rather than focusing only on illness or tasks.
Examples of Person-Centred Care in Practice
Understanding examples of person-centred care helps caregivers translate the theory into everyday practice. A strong person centred approach focuses on the individual’s preferences, routines, and goals rather than delivering identical care to every patient or resident.
Example 1: Dementia Care in a Care Home
A resident living with dementia becomes anxious in the evenings. Instead of applying a generic solution, resident site staff review the individual’s history and learn that the person previously worked night shifts. Caregivers adjust the routine, provide calming evening activities, and update the resident’s care plans to reflect this preference. This personalised adjustment reduces distress and improves wellbeing.
Example 2: Person-Centred Care in Nursing
In hospitals, examples of person-centred care in nursing often involve shared decision-making. A nurse explains treatment options to a patient recovering from surgery and asks about their comfort level, cultural needs, and recovery goals. The nurse then works with the patient to choose the most suitable care plan rather than making the decision alone.
Example 3: Domiciliary Care Support at Home
A domiciliary caregiver visits a client who values independence but needs help with daily activities. Instead of completing every task for them, the caregiver encourages the person to participate in preparing meals or organising medication. This person centred care approach supports independence while still ensuring safety and proper care.
These examples of person-centred care show how small adjustments in communication, planning, and daily support can significantly improve the quality of care in both healthcare and social care settings.
READ MORE: Do Dementia Sufferers Have to Pay Care Home Fees in the UK? (2026 Guide)
What Is Person-Centred Care and Why Is It Important?

Many caregivers ask what is person-centred care and why is it important in modern healthcare systems. The answer lies in how this approach improves both the experience and the outcomes of care. When professionals adopt a person centred approach, they move away from task-based care and focus on understanding the individual’s goals, values, and daily realities.
In care in health and social care, this approach builds stronger relationships between caregivers and the people they support. Patients and residents feel heard and respected, which increases trust and cooperation during treatment or support. As a result, individuals often follow care recommendations more confidently and remain more engaged in their own wellbeing.
Research also shows that patient centred care can lead to better health outcomes. When caregivers involve individuals in decisions, they often choose care options that align better with their lifestyle and needs. This improves satisfaction, reduces misunderstandings, and supports safer care delivery.
The importance of person centred care lies in recognising that healthcare is not only about treating illness. It is about supporting people to live meaningful lives while maintaining dignity, independence, and control over their own health decisions.
Benefits of Person-Centred Care for Patients and Caregivers
The benefits of person-centred care extend beyond improving patient satisfaction. When caregivers adopt a person centred approach, both individuals receiving care and the professionals delivering it experience better outcomes.
1. Improved Health Outcomes
When individuals participate in decisions about their treatment, they often follow care recommendations more consistently. This leads to better management of long-term conditions and fewer complications.
2. Greater Independence
Person centred care encourages people to maintain control over their daily lives. Caregivers support individuals in completing tasks themselves where possible, helping them build confidence and maintain independence.
3. Better Communication and Trust
Open conversations between caregivers and individuals strengthen relationships. Patients feel more comfortable sharing concerns, which helps caregivers provide safer and more effective care.
4. Higher Satisfaction for Patients and Staff
When care reflects a person’s preferences and goals, individuals feel respected and valued. Caregivers also experience greater job satisfaction because they see the positive impact of their work.
5. More Effective Care Planning
A person centred approach ensures that care plans reflect the individual’s real needs rather than generic assumptions. This leads to more coordinated support across healthcare and social care services.
Overall, the benefits of person-centred care include improved wellbeing, stronger relationships between caregivers and patients, and better long-term outcomes across care in health and social care settings.
SEE ALSO: Attendance Allowance Pitfalls (2026): Best Guide to Claim AA Successfully
What Is Person-Centred Planning?

Person-centred planning is the process caregivers use to turn the principles of person centred care into practical support. Instead of professionals creating plans alone, caregivers work with the individual, their family, and other professionals to design care plans that reflect the person’s goals, preferences, and daily life.
When people ask what is person centered planning, they usually want to understand how individuals stay involved in shaping their own care. In a person centred approach, planning begins with listening. Caregivers ask about what matters most to the person, how they want to live, and what support they need to remain safe and independent.
For example, a care worker supporting someone with mobility challenges may ask about the person’s daily routine, hobbies, and preferred level of assistance. The caregiver then adapts the care plans to support those activities rather than replacing them with a standard schedule.
In care in health and social care, effective person-centred planning helps coordinate services across nurses, support workers, therapists, and family members. When everyone works from the same personalised plan, care becomes more consistent, respectful, and aligned with the individual’s needs.
Person-Centred Care in Nursing and Therapy
Healthcare professionals apply person centred care every day in clinical settings. Nurses, therapists, and support workers use a person centred approach to understand the individual behind the condition and adapt care accordingly.
In nursing practice, examples of person-centred care in nursing often involve communication and shared decision-making. A nurse caring for a patient recovering from surgery may ask about the person’s pain tolerance, cultural preferences, and recovery goals before adjusting medication schedules or rehabilitation plans. Instead of delivering standardised treatment, the nurse works with the patient to create a recovery plan that suits their needs.
Mental health professionals also use person centred therapy, a psychological approach that focuses on empathy, active listening, and unconditional positive regard. Therapists encourage individuals to express their thoughts and feelings openly while guiding them to develop their own solutions to personal challenges.
Across care in health and social care, these approaches strengthen trust between professionals and individuals receiving support. When caregivers actively listen and respond to personal needs, they build stronger relationships and deliver care that respects dignity, independence, and individual identity.
MORE: Council Care Cost Inheritance: Who Pays for Care Home Fees 2026?
Key Takeaways
- Person centred care places the individual at the centre of all decisions about their health, wellbeing, and daily support. It focuses on understanding the person’s preferences, values, and goals rather than treating only a condition or illness.
- When people ask what is person centred care, the answer involves a collaborative approach where caregivers, patients, and families work together to shape support that reflects the individual’s needs.
- The four core principles of person centred care include respect and dignity, individualised support, shared decision-making, and empowerment to maintain independence.
- Real examples of person-centred care appear in everyday situations across care in health and social care, from nurses involving patients in treatment decisions to domiciliary caregivers adapting care plans to suit a person’s routine.
- The benefits of person-centred care include improved health outcomes, stronger caregiver-patient relationships, better communication, and greater independence for individuals receiving support.
By applying a consistent person centred approach, healthcare professionals and caregivers can deliver support that respects each individual’s identity, promotes wellbeing, and improves the overall quality of care.
Need Expert Guidance on Person-Centred Care?
Care Sync Experts supports care providers, managers, and healthcare teams across the UK with clear, practical guidance on delivering high-quality person centred care that meets regulatory expectations. From strengthening care plans and improving service quality to preparing for CQC inspections and embedding person-centred practices in daily care delivery, our team helps organisations build safer, more responsive care services.
Whether you need support training staff, reviewing care documentation, or aligning your service with modern health and social care standards, we provide structured, professional guidance you can trust.
Deliver care that truly puts people first.
Contact Care Sync Experts today and build a stronger, person-centred service with confidence.
FAQ
Which Best Describes Person-Centred Care?
The best description of person-centred care is an approach where healthcare professionals design care around the individual’s needs, preferences, and goals rather than focusing only on their illness.
Caregivers work in partnership with patients and their families to make decisions about treatment, support, and daily care. This approach ensures that care remains respectful, personalised, and responsive to each person’s unique situation.
What Are the 7 Person-Centred Care Values?
Many healthcare frameworks describe seven person-centred care values that guide how professionals should support individuals. These values include:
Individuality – recognising that every person has unique needs and preferences.
Rights – respecting each person’s legal and human rights.
Privacy – protecting personal space and confidential information.
Choice – allowing individuals to make decisions about their care.
Independence – supporting people to do as much for themselves as possible.
Dignity – treating every person with respect and compassion.
Partnership – involving families, caregivers, and professionals in collaborative care.
Together, these values help ensure that care remains respectful, empowering, and tailored to the individual.
What Are the Challenges of Person-Centred Care?
While person-centred care improves outcomes, caregivers often face challenges when applying it consistently. One common challenge is time pressure, especially in busy healthcare environments where staff must complete many tasks within limited time.
Another challenge involves communication barriers, such as language differences or cognitive conditions that make it harder to understand a person’s preferences.
Healthcare organisations may also struggle with resource limitations, including staffing shortages or limited training on person-centred practices. Overcoming these challenges requires strong leadership, continuous staff education, and systems that prioritise individual needs rather than rigid routines.
How to Show Person-Centred Care?
Caregivers demonstrate person-centred care through everyday actions that respect and involve the individual. This includes actively listening to the person, asking about their preferences, and involving them in decisions about treatment or support. Care providers should also adapt care plans to reflect the individual’s lifestyle, culture, and personal goals.
Simple actions, such as explaining procedures clearly, offering choices, and encouraging independence, help build trust and dignity. When caregivers consistently communicate with empathy and respect, they create an environment where individuals feel valued and supported in their health and well-being.

Leave a Reply